Reproductive Tissue Remodeling in Pregnancy
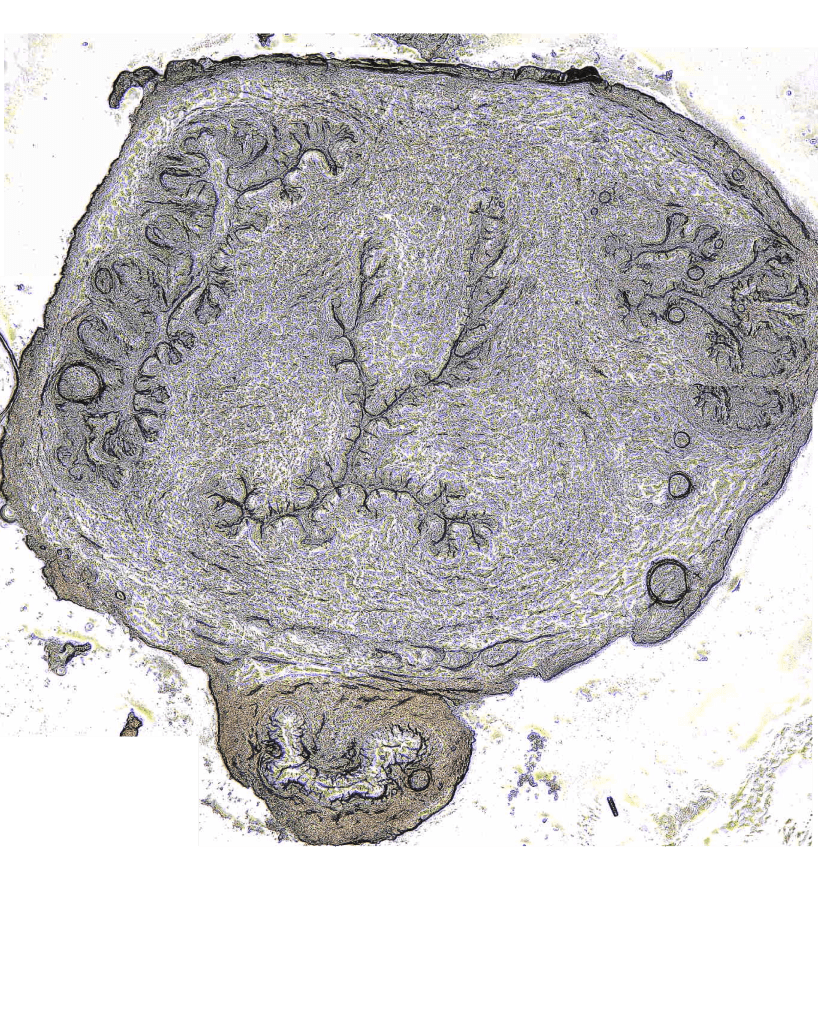
Mechanical Behavior of the Murine Cervix
The mouse model has been integral for studying the role of the extracellular matrix in cervical remodeling. The short gestation period and genetic tools have allowed the interrogation of remodeling at distinct gestation time points and the elucidation of the mechanical role of individual ECM components. The Myers lab seeks to characterize the complex hyperviscoelastic mechanical behavior of the cervix in healthy and disease models to discern material failure mechanisms related to preterm cervical remodeling and its contribution to preterm birth. This work is done in collaboration with Mala Mahendroo’s lab at the University of Texas Southwestern Medical Center (website).

Reproductive Tissue Remodeling During Pregnancy Using a Nonhuman Primate Model
We look at the material remodeling during pregnancy using a nonhuman primate model, where we combine optical imaging, mechanical testing, and computational modeling to investigate the evolution of tissue mechanical properties. This work is done in collaboration with Timothy J. Hall, Ivan Rosado-Mendez at the University of Wisconsin-Madison, Joy Vink at Hawaii Pacific Health, and Helen Feltovich at Intermountain Healthcare.
Mapping the Human Uterus
The uterus undergoes dramatic cellular and extracellular matrix growth and remodeling throughout the course of pregnancy and in the context of many gynecological diseases. We seek to characterize the multi-scale time-dependent mechanical properties of the uterus in healthy and pathological nonpregnant and pregnant states, utilizing nanoindentation, macro-scale indentation, and tensile testing.
Clinically Implementable Computational Tools

Ultrasound-based Models of Pregnancy
We have developed a novel solid modeling routine to generate parametric solid models of the pregnant abdomen based on maternal ultrasonic data. These models are used in finite element simulations to explore the biomechanical environment of pregnancy. Research thus far has revealed that maternal geometric and material properties of the cervix influence the distribution and magnitude of tissue stretch. We believe this predictive engineering analysis will provide a better understanding of how reproductive tissues are loaded in-vivo, shed light on tissue loading that could lead to preterm delivery, and guide the development of patient-specific therapeutic interventions.
Clinical Studies
We have several observational clinical studies underway with our collaborators at CUIMC to investigate how the uterus and cervix grow and remodel during pregnancies at high- and low risk for preterm birth. These studies are also used to develop and validate our engineering workflow.
Characterizing Low-Risk Pregnancies
We are currently measuring time-course maternal and fetal anatomy and cervical tissue properties throughout gestation. Using these measurements we are building patient-specific FEA models to establish tissue stress and stretch profiles throughout human pregnancy.
Mechanical Function of Pessary
We are participating in an ancillary study to the NICHD Maternal-Fetal Medicine Units (MFMU) Network TOPS trial, evaluating the mechanical benefit of the pessary for singleton pregnancies. Our study will build FEA models of subjects with and without pessary to calculate and visualize the pattern and magnitude of cervical stress and stretch. We will evaluate birthing outcomes as a function of the mechanical loading environment.
Patients with a History of Preterm Delivery
Since those who are at greatest risk of delivering preterm are patients who have delivered prematurely in previous pregnancies, we are currently collecting transvaginal ultrasounds and cervical stiffness measurements of patients with a history of preterm birth. This case population will help characterize cervices at the highest risk of preterm birth.
Funding Agencies
National Institutes of Health – NICHD
National Science Foundation – CMMI
Columbia University Irving Institute for Clinical and Translational Medicine
March of Dimes Prematurity Research Center – University of Pennsylvania
The Iris Fund
